ChartFlow Team
The Simulation Gap Most Nursing Programs Don't Know They Have
Your simulation lab is impressive. You've invested in high-fidelity manikins, built standardized patient scenarios, maybe even explored VR headsets. Students practice auscultating lung sounds, managing IV lines, and responding to rapid deterioration — all before touching a real patient.
But here's the question most simulation coordinators haven't asked: What happens when your student sits down at the computer in their first clinical rotation?
In every hospital, clinic, and long-term care facility in the United States, clinical documentation happens inside an electronic health record. Documentation errors, EHR navigation struggles, and charting delays are consistently cited as contributors to adverse events, medication errors, and communication failures. Yet the vast majority of nursing programs send students into clinical rotations having never once practiced inside a realistic EHR environment.
This is the simulation gap — and it's hiding in plain sight.
Modern nursing simulation software has expanded well beyond manikins and task trainers. EHR simulation platforms now make it possible to give every student hundreds of hours of clinical documentation experience before they ever log into a hospital system. This guide explains what's available, why it matters, and how to build a complete simulation curriculum that actually prepares students for the job.
The Nursing Simulation Landscape in 2026
Nursing simulation is not one thing. It's a spectrum of modalities, each addressing different competency domains. Understanding the full landscape helps programs make intentional decisions — and spot the gaps.
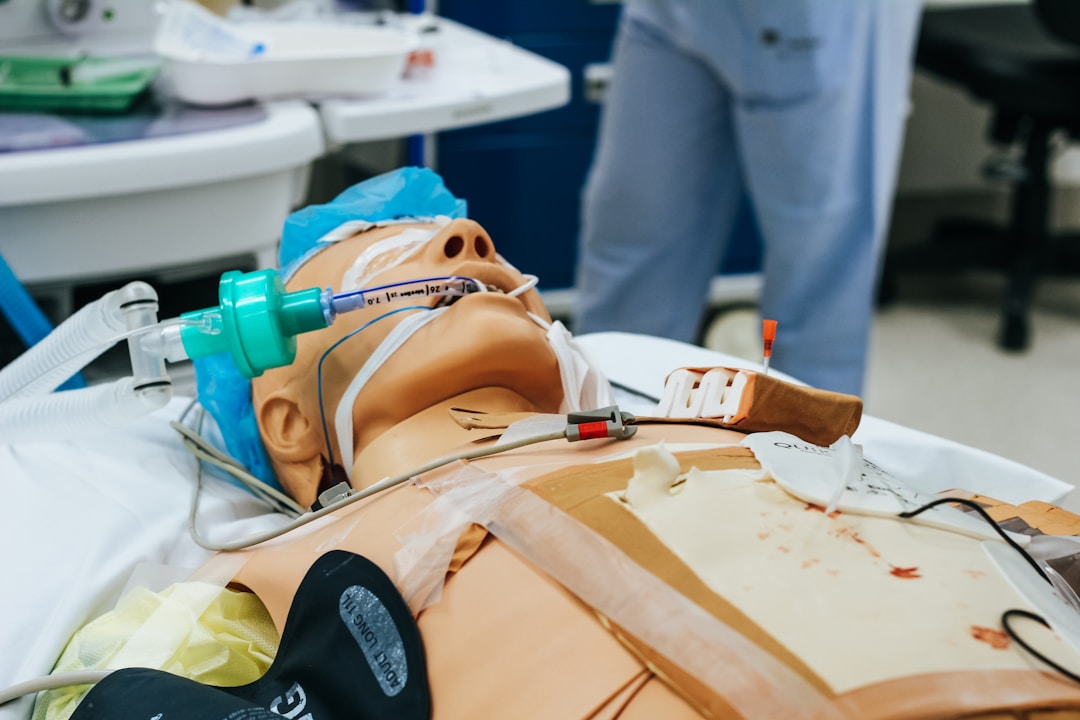
High-Fidelity Manikins
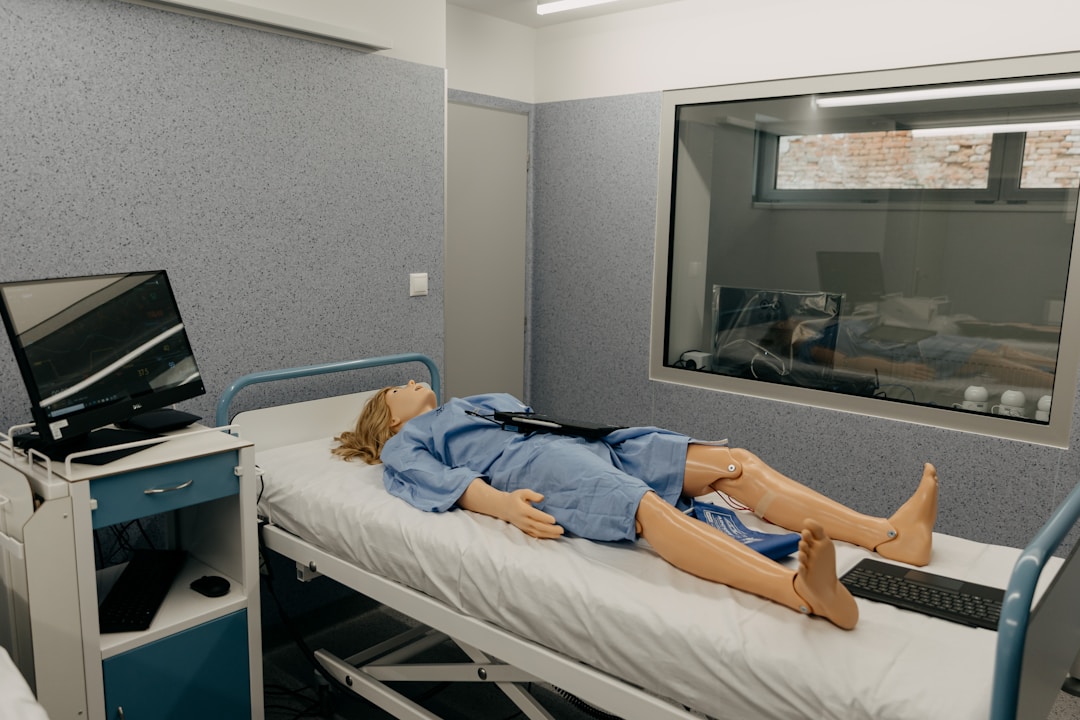
The cornerstone of most simulation programs. Manikins like those from Laerdal, CAE, and Gaumard can breathe, respond to medications, generate vital signs, and simulate childbirth. They're unmatched for procedural skills, emergency response, and developing clinical judgment in high-acuity scenarios.
- Strengths: Hands-on psychomotor skill development, teamwork, SBAR communication, rapid-response training.
- Limitations: Expensive (often $30K–$100K+ per unit), requires trained simulation technicians, and addresses almost no informatics competencies.
Virtual Reality (VR) Simulation
VR platforms like Oxford Medical Simulation and Schwartz/Rounds VR bring immersive patient encounters into a headset. Students can practice therapeutic communication, patient assessment, and clinical reasoning in simulated ward environments.
- Strengths: Scalable, accessible, increasingly realistic.
- Limitations: Still maturing in nursing education, high hardware cost, and generally does not address clinical documentation.
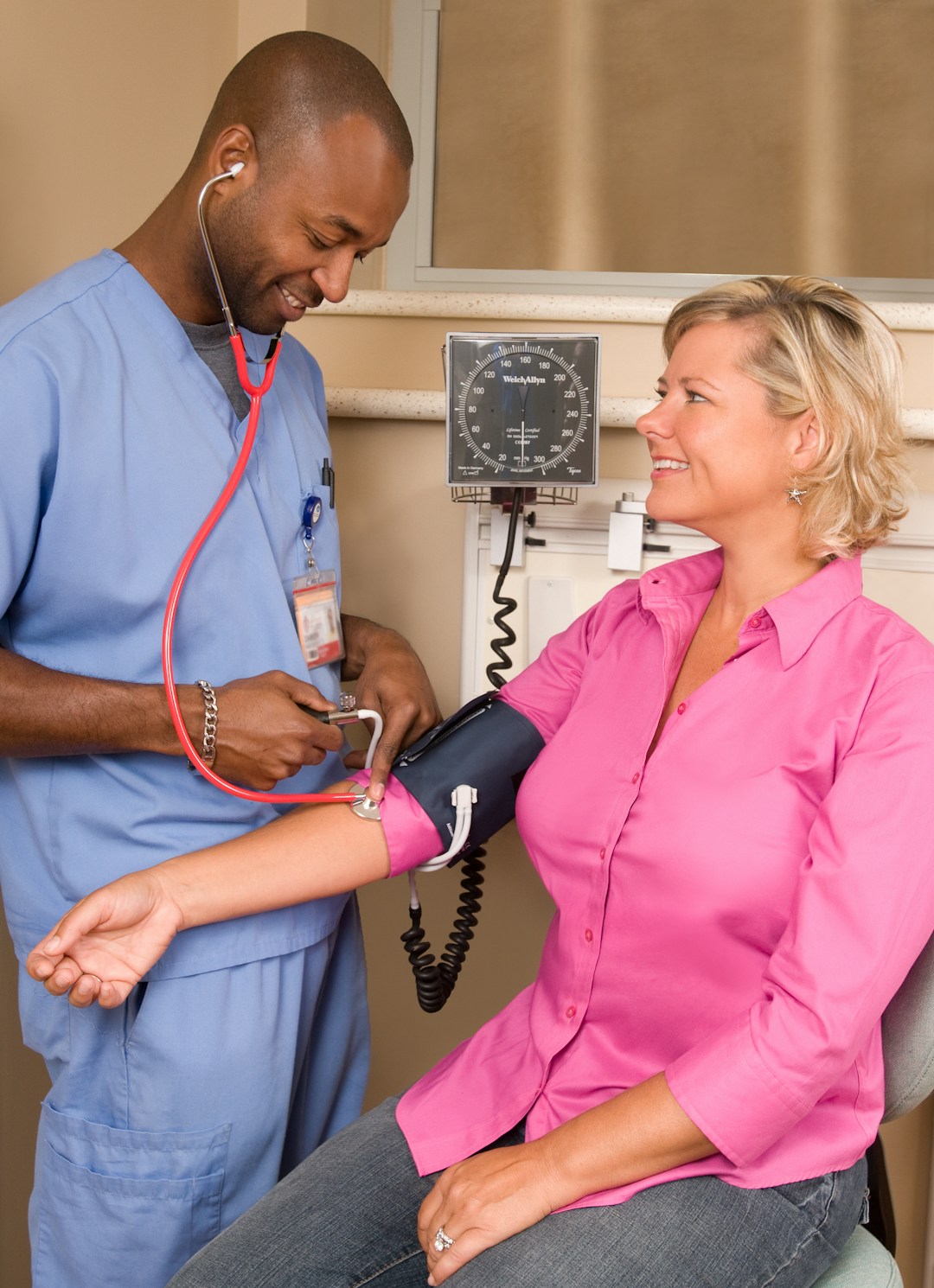
Standardized Patients (SPs)
Trained actors portraying patients allow students to practice communication, physical assessment, and empathy in a realistic interpersonal context. Standardized patients are invaluable for OSCE (Objective Structured Clinical Examination) preparation.
- Strengths: Human interaction, nuanced communication training, ideal for difficult conversations.
- Limitations: Scheduling complexity, faculty time, and no EHR documentation component.
EHR Simulation Software
Simulated EHR platforms replicate the electronic health record environment students will encounter in clinical settings. Students practice nursing assessments, medication administration records (MAR), care planning, SBAR handoff documentation, and clinical decision-making — all within a realistic charting interface.
- Strengths: Directly addresses QSEN informatics competencies, prepares students for actual clinical workflows, scalable at low cost, easily integrated with existing curricula.
- Limitations: Less tactile than manikin simulation; best used in combination with other modalities.
Why EHR Simulation Is the Missing Piece
The QSEN Imperative
The Quality and Safety Education for Nurses (QSEN) framework identifies Informatics as one of six core competency domains that all prelicensure nurses must develop. Specifically, QSEN calls for nurses to:
"Use information and technology to communicate, manage knowledge, mitigate error, and support decision making."
The 2021 AACN Essentials reinforce this, embedding informatics and healthcare technology throughout their ten domains — including explicit language around clinical documentation, decision support tools, and interoperability.
When your program doesn't include structured EHR training, you're leaving a QSEN competency domain largely unaddressed. Accreditation bodies are paying closer attention to this. ACEN and CCNE site visitors increasingly ask programs how they are addressing informatics competencies in their curriculum mapping. A simulated EHR, documented in your curriculum maps, is a concrete, defensible answer.
Clinical Readiness: What the Research Shows
The evidence is consistent: students who arrive at clinical rotations without EHR experience take longer to become functional, make more documentation errors, and report higher anxiety around charting tasks. Preceptors — already stretched thin — spend significant time teaching EHR navigation instead of clinical reasoning.
The NCLEX Connection
The 2023 Next Generation NCLEX (NGN) emphasizes clinical judgment across complex, multi-step scenarios. Many NGN item types — including matrix items and extended multiple response — require students to interpret and act on information presented in EHR-style formats: progress notes, lab results, MAR entries, provider orders.
EHR for nursing students isn't just about documentation — it's about reading and synthesizing charted information to make sound clinical decisions. Programs that use simulated EHR platforms are, incidentally, also preparing students for the cognitive demands of NGN-style items.
What to Look for in EHR Simulation Software
Not all simulated EHR platforms are created equal. Here's what to evaluate when selecting nursing simulation software for your program:
Realistic Charting Interface
The EHR should look and feel like actual clinical systems. If students are charting in a grid that barely resembles Epic or Cerner, the transfer of learning is limited. Look for platforms with structured assessments, flowsheets, MAR functionality, provider orders, and progress note templates that mirror real-world documentation workflows.
Pre-Built Patient Templates and Scenarios
Faculty time is precious. The best platforms include a library of patient cases — medical, surgical, pediatric, OB — that instructors can assign without building from scratch. The ability to customize cases is a bonus, but the out-of-the-box library matters.
Automated Grading and Faculty Feedback Tools
Manual chart review at scale is unsustainable. Look for platforms that offer automated grading rubrics, completion tracking, and faculty annotation tools. Integration with your LMS (Canvas, Blackboard, Moodle) for gradebook sync is a significant workflow advantage.
Affordability and Access Model
Simulation budgets are tight. Many programs can't justify per-seat costs at the same level as high-fidelity manikins. Look for platforms with reasonable per-student pricing (under $20/student is viable for most programs) and free instructor accounts — faculty shouldn't need to consume a student license just to set up and review assignments.
Ease of Implementation
The best tool is the one your faculty will actually use. Platforms that require extensive IT involvement, custom server setup, or weeks of onboarding training will stall adoption. Cloud-based, browser-accessible platforms with modern interfaces and clear faculty support resources are more likely to get embedded in curricula and stay there.
LMS and Curriculum Integration
A simulated EHR that lives in its own silo creates extra work. The strongest platforms offer LMS integration (via LTI or direct gradebook sync), embeddable links, and assignment structures that fit naturally into how your courses are already organized.
EHR Simulation Software: A Comparison for 2026
Several platforms serve the educational EHR simulation market. Here's an honest look at the major options:
ChartFlow
ChartFlow is a modern, web-based EHR simulation platform built specifically for nursing education. It features a clean, intuitive interface that students navigate without a learning curve, realistic patient charting workflows, activity-based assignments, and automated grading.
- Strengths: Modern interface, very easy for both faculty and students to use, free instructor accounts, competitive student pricing (~$15/student), responsive support, continuous improvement based on faculty feedback.
- Best for: Programs that want fast implementation, modern UX, and fair pricing without sacrificing realism or pedagogical depth.
EHR Go
EHR Go is one of the more established players in the educational EHR space, with a broad case library and multi-disciplinary support (nursing, pharmacy, allied health).
- Strengths: Large existing case library, multi-discipline support.
- Considerations: Interface can feel dated compared to newer platforms; pricing is higher and instructor accounts may require additional seats.
Elsevier SimChart
SimChart for the Medical Office is Elsevier's EHR simulation product, often bundled with Elsevier textbook adoptions.
- Strengths: Integration with Elsevier content ecosystem, familiar to programs already using Evolve.
- Considerations: Most cost-effective when bundled with existing Elsevier adoptions; standalone pricing is higher; primarily optimized for ambulatory/medical office workflows.
Wolters Kluwer DocuCare
DocuCare is Wolters Kluwer's simulated EHR, often paired with Lippincott content.
- Strengths: Integration with Lippincott/Lippincott Advisor content, familiar to programs in the Wolters Kluwer ecosystem.
- Considerations: Most valuable within the publisher's broader content bundle; standalone adoption carries higher cost and switching friction.
How to Implement EHR Training in Your Curriculum
Adding EHR simulation doesn't mean rebuilding your curriculum. Here's a practical implementation framework:
Start in Fundamentals
Introduce the simulated EHR in NUR 101 or equivalent. Use simple patient scenarios focused on basic nursing assessments, vital sign documentation, and intake/output. The goal isn't complexity — it's familiarity. Students need to know where to click before they're asked to think critically about what to document.
Layer Complexity with Clinical Coursework
As students progress through med-surg, pharmacology, and specialty rotations, assign EHR activities that match the clinical content. A med-surg student should be charting on a post-op patient with complex medication orders. An OB student should be completing labor and delivery documentation. The simulated EHR becomes a thread that runs through the entire curriculum.
Use EHR Scenarios as Pre-Clinical Preparation
Assign relevant EHR activities before each clinical rotation block. A student heading to their first ICU rotation should chart on a ventilated patient in the simulated EHR first. Arrive oriented, not overwhelmed.
Integrate with Simulation Lab Scenarios
The most powerful integration: run a manikin simulation, then require students to complete the documentation in the EHR platform afterward. This closes the loop — assessment → intervention → documentation — and mirrors real clinical workflow. Debrief both the clinical and documentation components.
Assess and Grade Like It Matters
Don't assign EHR activities as optional or ungraded. If it's not graded, students won't prioritize it. Build charting assignments into your clinical evaluation frameworks. Use the platform's grading tools to provide meaningful feedback, not just completion credit.
Prepare Faculty First
Faculty adoption is the rate-limiting factor in any simulation program. Schedule a faculty development session before launching — most modern platforms can be learned in under an hour. Designate a simulation champion who can support colleagues. Share the QSEN and AACN Essentials rationale so faculty understand why this belongs in the curriculum, not just what it is.
The Bottom Line
Nursing education has come a long way in simulation. High-fidelity manikins, standardized patients, and VR have transformed clinical preparation. But the electronic health record — the primary tool of modern nursing practice — has been largely absent from the simulation equation.
That's changing. Programs that build EHR simulation into their curricula produce graduates who arrive at clinical orientations ready to chart, ready to document, and ready to be functional members of a clinical team on day one. They demonstrate measurable informatics competency — a growing expectation from accreditors, healthcare employers, and the NCLEX itself.
EHR simulation isn't a replacement for any existing modality. It's the missing piece that completes the simulation ecosystem your program has been building.
Try ChartFlow — Free for Instructors
ChartFlow offers free instructor accounts with no time limit. You can build courses, assign patient scenarios, and experience the platform exactly as your students will — before committing to anything.
If you're ready to close the EHR simulation gap in your program, start there.
Q is the QA lead at ChartFlow.io, with a background in clinical nursing and nursing education. She focuses on making sure ChartFlow actually works the way nurses think — not just the way developers build.
More posts like this


















_(2)/w=1920,quality=90,fit=scale-down)






/w=1920,quality=90,fit=scale-down)









































/w=1920,quality=90,fit=scale-down)
_(1)/w=1920,quality=90,fit=scale-down)




















/w=1920,quality=90,fit=scale-down)