ChartFlow Team
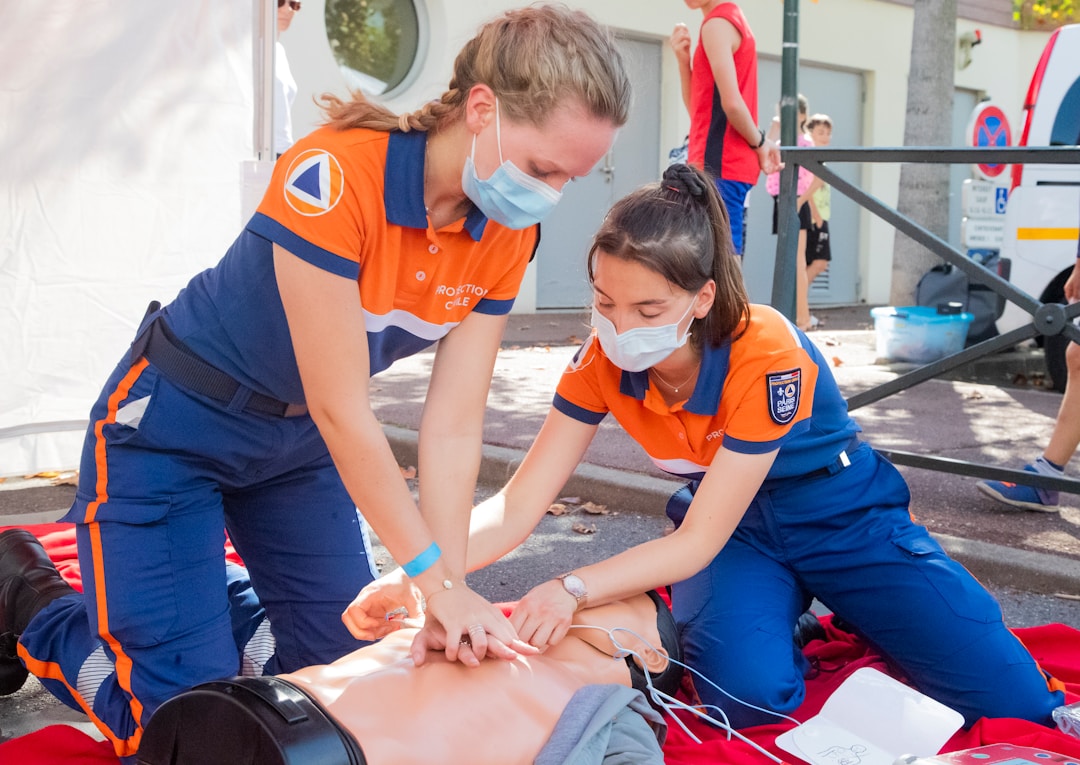
Your students can start an IV, perform a head-to-toe assessment, and manage a simulated code blue. But can they document it?
For most healthcare programs, EHR training is an afterthought — something students figure out on their first clinical rotation, standing at a workstation with a preceptor waiting behind them. That's not a skills gap. It's a curriculum gap. And it's one programs can close.
Why EHR Training Is No Longer Optional
The expectation is clear. The AACN Essentials (2021) identifies informatics and healthcare technologies as a core domain for professional nursing practice. QSEN's informatics competency requires that graduates use information and technology to communicate, manage knowledge, and support decision-making.
These aren't aspirational standards. Accreditors are asking about them. Clinical sites expect them.
Beyond accreditation, the reality is this: documentation is where errors occur. Medication reconciliation, allergy flags, intake and output, care plan entries — a student who doesn't know how to navigate an EHR is a liability risk during clinical rotations, and they know it. The anxiety alone affects performance.
EHR competency isn't a bonus skill. It's a core competency.
The Gap Most Programs Haven't Fixed
Here's the honest picture: the majority of nursing and allied health programs still treat EHR training as an orientation item, not a curriculum thread.
Students get a 30-minute walkthrough of how to log in. Maybe a demo of medication administration documentation. Then they're expected to chart real patients on real systems — Epic®, Cerner®, MEDITECH® — with minimal preparation.
The problem isn't that students are incapable. It's that they've never had the chance to practice.
Clinical simulation has solved this problem for hands-on skills. Manikins exist so students can practice central line dressing changes before touching a patient. The same logic applies to documentation: students need a safe space to fail, practice, and build fluency before it counts.
Most programs don't offer that. Not because they don't see the need — they do — but because building EHR training into a curriculum feels technically complicated, expensive, or or technologically impossible.
It doesn't have to be any of those things.
What Good EHR Training Actually Looks Like
Effective EHR training for healthcare students isn't about teaching them one vendor's proprietary system. It's about building transferable documentation skills: clinical reasoning translated into structured charting.
Here's what that looks like in practice:
It starts with the scenario, not the software.
Students should encounter a patient — history, presenting complaint, vitals, lab results — and document what they observe and decide. The EHR is the medium, not the focus. The focus is clinical thinking.
It runs alongside simulation, not after it.
The highest-value integration pairs hands-on simulation with documentation. Students perform a patient assessment on a manikin, then immediately document their findings in a simulated EHR. That workflow mirrors real clinical practice and reinforces both skills simultaneously.
It's iterative, not one-and-done.
A single EHR lab in week two of the semester doesn't build competency. Documentation practice should be woven into case-based learning throughout the program — across courses, across semesters, building complexity as students advance.
It uses realistic, customizable patient cases.
Generic placeholder patients don't teach clinical judgment. Students need cases that reflect the patients they'll actually see: a 67-year-old with CHF and a history of non-compliance, a post-op patient three hours out of surgery, a pediatric case with weight-based dosing. The more realistic the case, the more transferable the skill.
It gives instructors visibility.
If an instructor can't see what a student documented, they can't give feedback. EHR training that happens in a black box — no review, no correction — doesn't improve practice. It just builds bad habits faster.
How ChartFlow Fits Into This
ChartFlow is a browser-based EHR simulation platform built specifically for healthcare education programs. It's designed to be used exactly the way good EHR training should be used: embedded in curriculum, paired with simulation, and accessible on all devices (phones, tablets, laptops, desktops, Chromebooks, etc.)
A few things that matter for program directors evaluating options:
Instructor accounts are free.
You can build out a course, create patient templates, and assign activities without spending a dollar. Student access runs around $15 per student — less than a clinical textbook.
It runs in a browser.
No software to install, no server to maintain, no IT ticket required. Students access it from any device. You can run a documentation lab in a computer room, have students complete charting homework from home, or integrate it into your existing LMS workflow through an LTI 1.3 integration.
Patient templates are customizable.
You build the patient. You control the history, the vitals, the medications, the lab values, the clinical context. A med-surg faculty member can build different patients than the OB faculty. A paramedic program can create pre-hospital scenarios. The platform adapts to your curriculum, not the other way around.
It works alongside your existing simulation.
ChartFlow isn't a replacement for your manikins or your standardized patients. It's the documentation component that most simulation programs are missing. Run the physical scenario first, then have students sit down and chart what just happened. That's the workflow.
Instructors can review student documentation.
You can see what students entered, identify errors in clinical reasoning, and give targeted feedback. Documentation review becomes part of the debrief, not a separate process.
Where to Start
The barrier to integrating EHR training isn't budget or technology. It's activation energy — deciding to start.
Here's a low-lift entry point: pick one existing simulation scenario your students already run. After the debrief, have students open ChartFlow and document the encounter. One assessment note. One set of vitals. That's it.
Watch what happens. Most students will slow down, realize they don't have the language, and start asking questions they've never asked before. What do I call this finding? Where does this go? How do I document a refusal?
Those questions are the point. The EHR surfaces gaps in clinical vocabulary and documentation reasoning that physical simulation doesn't catch. Better to find those gaps in your lab than at the clinical site.
From there, you can build. Add medication documentation. Add care planning. Add complex cases with abnormal labs that require follow-up. Over a semester, students build genuine fluency — not just familiarity.
The Students Who Walk In Ready
There's a version of your graduates who sit down at the clinical workstation and know what they're doing. Who can navigate a chart, document an assessment, and flag a discrepancy — without freezing, without asking their preceptor to walk them through it, without that first week of playing catch-up.
That version of your graduates exists. It just requires treating documentation as a skill that's taught, practiced, and assessed — the same way you treat every other clinical skill.
EHR training for healthcare students isn't a technology problem. It's a curriculum decision.
Ready to see how ChartFlow fits your program?
Instructor accounts are free. No demo call required — you can build your first activity today at chartflow.io.
More posts like this


















_(2)/w=1920,quality=90,fit=scale-down)






/w=1920,quality=90,fit=scale-down)









































/w=1920,quality=90,fit=scale-down)
_(1)/w=1920,quality=90,fit=scale-down)




















/w=1920,quality=90,fit=scale-down)